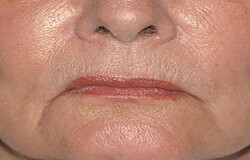
A 70-year-old patient presents complaining of persistent soreness and cracking at the corners of her mouth, along with intermittent numbness of the lower lip and chin. Symptoms are more noticeable during prolonged denture wear.
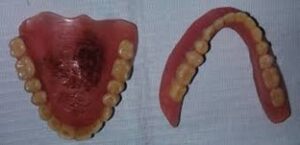
She has worn complete dentures for many years and reports that her mandibular denture feels loose and unstable, rocking during function. She maintains good denture hygiene and removes her dentures overnight.
Medical history includes type 2 diabetes mellitus and hypertension, both medically managed. She does not smoke and drinks alcohol occasionally.
On examination, there is bilateral erythema and fissuring at the oral commissures with mild maceration. The mandibular denture shows reduced stability and loss of support.
You decide to reline the mandibular denture to improve fit and support.
At review four weeks later, the patient reports that the corner-of-mouth irritation has significantly improved, but the lower lip and chin numbness persists.
Q1. At the initial presentation, what was the PRIMARY factor to the angular cheilitis in this case?